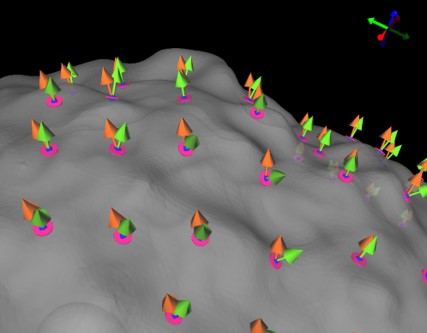
Neural Effects of Electrical Stimulation in Computational Models
We build multiscale computational models of neural activation in Deep Brain Stimulation (DBS) therapy. DBS is a clinically used and widely effective treatment for the symptoms of Parkinson's disease, essential tremor, and other neurological disorders. However, which neurons and neural regions are activated by DBS is not presently understood. With our biophysical computational models -- scaling from individual neurons to the entire brain -- we aim to understand how electric fields modulate neural activity, and to develop precise constraints that clinicians could use to optimally target neural structures.
Patient-Specific Neuromodulatory Data Analysis
We utilize advanced data analysis and computational approaches to evaluate neural activity and clinical outcomes in patients receiving neuromodulation therapy. While invasive neuromodulation provides significant symptomatic relief, the optimal stimulation parameters vary across individuals and over time. Using clinical datasets—including intraoperative recordings and chronic sensing from responsive neurostimulation systems—we validate patient-specific biomarkers and characterize the structural connectivity that informs therapeutic success. By integrating these longitudinal data, we aim to develop automated tuning algorithms and visualization tools that assist clinicians in identifying the most effective, personalized stimulation protocols for managing neurological diseases.